The link Between Age-related macular degeneration (AMD) and Ethnicity.
Genetics has the power to unlock the mysteries of our physical traits, our predisposition to disease and even our evolutionary history. In fact, AMD is caused by genetic factors and environmental. AMD is a leading cause of vision loss and blindness, particularly among the elderly population. While various factors contribute to the development and progression of AMD, emerging research suggests that ethnicity may also play a role in influencing the risk and characteristics of the disease.

Understanding AMD
AMD is a degenerative disease that affects the macula, a small area of the retina responsible for central vision and the perception of fine detail. AMD is the leading cause of vision loss in people over 50. It is divided into two main forms: dry AMD, which progresses slowly, and wet AMD, which is more severe and progresses rapidly. Common risk factors for AMD include age, heredity, smoking, exposure to ultraviolet radiation, a diet low in antioxidants and certain cardiovascular problems.
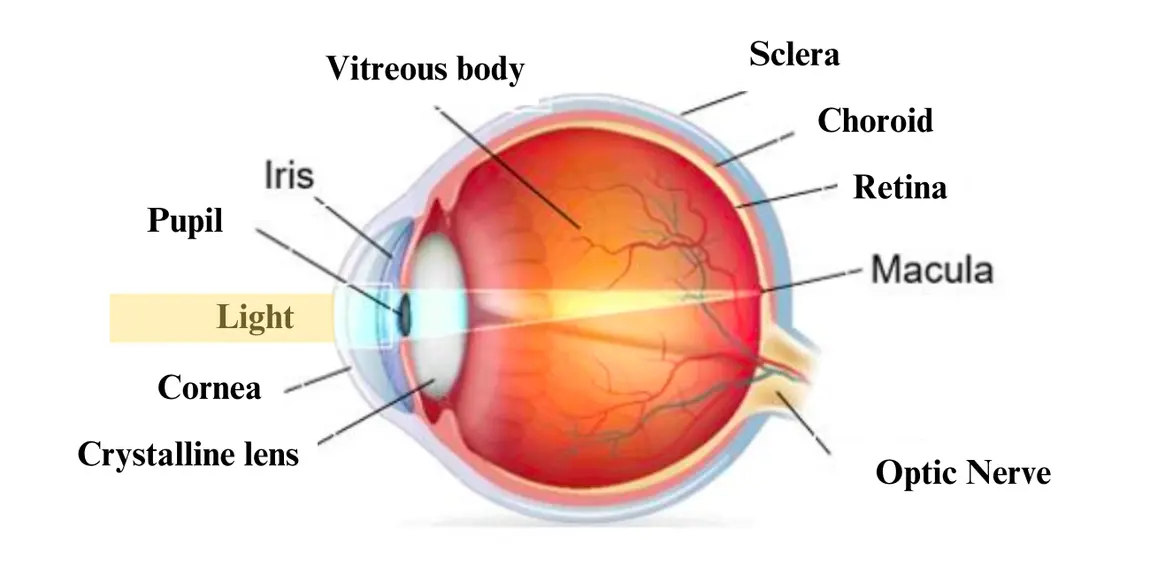
Figure 1. Anatomy of the human eye
The occurrence, characteristics, and changes of AMD differ among different ethnic groups. Many studies have shown that ethnic background influences the likelihood of developing AMD, indicating that genetic and environmental factors may play a role.
Ethnic origin can influence a person's genetic profile and their chances of developing AMD.
We have published another article where you can learn more about AMD and its risk factors.
Ethnicity and Genetic Factors
Having certain genes makes a person more likely to develop AMD, and these genes can differ between ethnic groups.
For example, in Caucasian populations, a specific version of the complement factor H (CFH) gene has been linked to a higher risk of AMD.
On the other hand, individuals of Asian descent tend to have a higher occurrence of the ARMS2 gene variant.

Figure 2.Ethnic origin influences genetic profile
Ethnicity can affect a person's genetic profile and their chances of developing AMD.
Ethnicity and Environmental Factors
Apart from genetic factors, environmental and lifestyle influences may also interact with ethnicity to impact AMD risk. Dietary habits, sun exposure, smoking, and other lifestyle choices can vary across ethnicities, potentially influencing the development and progression of AMD. For example, diets rich in antioxidants and Omega-3 fatty acids, common in certain ethnic cuisines (Mediterranean diet ), have been associated with a lower risk of AMD. Conversely, higher rates of smoking in some ethnic populations may contribute to an increased risk of the disease.

Figure 5 Mediterranean diet pyramid
Clinical Features and Progression
Studies have found that AMD behaves differently among various ethnic groups. For example, people of Asian descent tend to have a higher chance of developing a specific type of wet AMD called polypoidal choroidal vasculopathy (PCV). In PCV, abnormal blood vessels grow under the retina, leading to vision problems.
Furthermore, the age at which AMD begins and the speed at which it progresses can differ among ethnicities. This highlights the importance of tailoring management strategies to each person.
Implications for Disease Management
Understanding how ethnicity influences AMD highlights the need for personalized screening and early intervention. Also, personalized treatment approaches that account for both genetic and environmental factors can maximize the effectiveness of therapy. By customizing interventions based on an individual's genetic predisposition and lifestyle choices, better management of AMD can be achieved.
Conclusion
Understanding the relationship between AMD and ethnicity is a complex and evolving area of research. While ethnicity alone cannot solely predict an individual's risk of developing AMD, it represents an important factor that interacts with genetics, lifestyle, and environmental influences. Further studies focusing on diverse ethnic populations are crucial to unravel the underlying mechanisms and optimize AMD prevention, diagnosis, and treatment strategies for different groups.
You can also have access to personalized lifestyle recommendations to prevent AMD by visiting www.macutest.com.
Bibliography
- T. J. Heesterbeek, L. Lorés-Motta, C. B. Hoyng, Y. T. E. Lechanteur, et A. I. D. Hollander, « Risk factors for progression of age‐related macular degeneration » , Ophthalmic and Physiological Optics, févr. 2020.
- « Age-Related Macular Degeneration (AMD) | National Eye Institute » .
- *What Is Macular Degeneration ?* (2023, 6 avril). American Academy of Ophthalmology.
- D. O. Fisher et al., « Incidence of Age-Related Macular Degeneration in a Multi-Ethnic United States Population » , Ophthalmology, juin 2016.
- Bryn Mawr Communications, « Prevalence of AMD in Whites, Blacks, Hispanics and Chinese - Retina Today » , Retina Today.
- B. L. VanderBeek, D. N. Zacks, N. Talwar, B. Nan, D. C. Musch, et J. D. Stein, « Racial Differences in Age-Related Macular Degeneration Rates in the United States : A Longitudinal Analysis of a Managed Care Network » , American Journal of Ophthalmology, août 2011.
- Y.-H. Chen, M. Bedell, et K. Zhang, « Age-related Macular Degeneration : Genetic and Environmental Factors of Disease » ,2010.
- « Genetics and Age-Related Macular Degeneration » , American Academy of Ophthalmology, 17 mars 2023.
- R. Klein et al., « Prevalence of Age-Related Macular Degeneration in 4 Racial/Ethnic Groups in the Multi-ethnic Study of Atherosclerosis » , Ophthalmology, mars 2006.
- Addo, E. K., Hartnett, M. E., & Bernstein, P. S. (2023). The value of pre-symptomatic genetic risk assessment for age-related macular degeneration.
Ultraviolet aggravate age related macular degeneration (AMD)
We all love to enjoy the sun's rays. However, it is important to remember that excessive exposure to the sun and ultraviolet (UV) rays can have a harmful impact on our eyes. The UV rays emitted by the sun can cause invisible but significant damage to our eyes, leading to long-term vision problems. They can aggravate eye diseases such as cataracts and AMD.
Exploring Gender Differences in Age-Related Macular Degeneration (AMD)
GAMD is a progressive eye disease affecting millions of people worldwide. Although AMD is known to be more common in older people, it is possible to determine whether gender influences the progression and treatment of AMD.